Diabetes
The Facts about Diabetes

What is diabetes?
Diabetes is a chronic disease that affects how your body turns food into energy. Most of the food you eat is broken down into glucose (sugar) and is released into your bloodstream to be used by your cells for energy.
When you consume food, your blood sugar goes up. This rise in blood sugar normally signals your pancreas to release insulin, a hormone that acts like a key to let the blood sugar leave your bloodstream and enter your body’s cells. Insulin helps control your blood glucose level to keep it in a healthy range.
If you are diabetic, however, your body typically 1) does not make any insulin 2) doies not make enough insulin, or 3) cannot use the insulin your pancreas produces as well as it should.
When there is not enough insulin in your body, or your cells stop responding to insulin, too much blood sugar remains in your bloodstream and your blood sugar levels get too high. Over time, this consistently high level can damage body organs and cause serious health problems such as heart disease, kidney disease, and loss of vision, among other complications.
There are three main categories of diabetes. While all three share the characteristic of high blood glucose (sugar) levels in the blood, there are notable differences with each type.
The 3 main types of diabetes
The three main types of diabetes are type 1, type 2, and gestational diabetes (diabetes during pregnancy). Type 2 is the most common form of diabetes and is reversible , so we will begin by explaining type 2.
Type 2 Diabetes
Type 2 diabetes occurs when your body does not use the insulin your pancreas produces effectively. Your body is not able to keep blood sugars at normal, desirable levels. About 90-95% of people with diabetes have type 2 diabetes. Unlike type 1, type 2 develops over many years, not suddenly. In the past, type 2 diabetes was usually an adult disease. Today, however, more and more children, teens, and young adults are being diagnosed with type 2 diabetes due to lifestyle habits and other variables.
Symptoms of type 2 diabetes may not appear for a long time. There may be no signs for years. Therefore, it is important to get your blood sugar tested if you are at risk. Type 2 diabetes can be prevented, delayed, or even reversed with healthy lifestyle changes, such as weight loss, exercise, and a healthy diet.

Type 1 Diabetes
Type 1 diabetes is believed to be caused by an autoimmune reaction (the body’s immune system attacking itself by mistake). With type 1 diabetes, T cells attack the beta cells in the pancreas, destroying the body’s ability to produce insulin. Without insulin, glucose (sugar in the blood) cannot enter cells to produce energy. The symptoms of type 1 diabetes often develop suddenly and include chronic thirst, frequent urination, blurry vision, deep fatigue, or life-threatening diabetic ketoacidosis.
Left untreated, type 1 diabetes can cause dehydration, weight loss, nerve and blood vessel damage, organ damage, and life-threatening diabetic ketoacidosis (DKA). DKA is a serious complication of diabetes that occurs when the body produces high levels of blood acids called ketones as a result of low insulin levels. In the case of DKA, immediate hospitalization is needed.
Only 5-10% of people with diabetes have type 1. This type of diabetes usually strikes babies, children, teens, and young adults. Although much less common, type 1 can also appear in older adults.
Individuals with type 1 diabetes need to take insulin every day. The injected insulin does what the pancreas can no longer do: help the body use sugar that is in the bloodstream. Without insulin, the body can quickly develop hypoglycemia (too much blood sugar) which, if not medically addressed, can lead to DKA and be fatal.
Currently, there are no known ways to prevent type 1 diabetes. But with advances in medicines and medical technologies, type 1 diabetics now have many different options for insulin delivery and glucose level monitoring and management. There are insulin pumps that provide continuous glucose monitoring and a steady supply of insulin drip. There are short-acting and long-acting insulins, blood testers, and other medical aids. Your healthcare provider will talk with you about what diabetic tools work best with your lifestyle to meet your ongoing daily need to manage your diabetes to the best of your ability.
The daily use of insulin and the daily monitoring of glucose levels in the blood, allow type 1 diabetics to manage hypoglycemia (dangerously low blood sugar level) and hyperglycemia (dangerously high blood sugar level). The symptoms for each of these conditions, include the following:

Gestational Diabetes
Gestational diabetes develops during pregnancy in women who may have never had diabetes. If gestational diabetes develops during pregnancy, your baby could be at higher risk for certain health problems. Gestational diabetes usually goes away after your baby is born, but having gestational diabetes while pregnant, does, unfortunately, increase your risk for type 2 diabetes later in life. Also, your baby is more at risk for becoming obese as a child or teen, and for developing type 2 diabetes later in life, too.

What are the signs and symptoms of diabetes?
If you have any of the following diabetes symptoms, see your healthcare provider to get your blood sugar level tested:
- Need to urinate (pee) a lot, getting up a lot at night to pee, or are wetting your bed unknowingly
- Feel unusually thirsty and hungry throughout the day
- Are losing weight without trying
- Experiencing blurry vision
- Have numbness or tingling in your hands or feet
- Feeling generally very tired, deep fatigue
- Have very dry skin
- Have sores that are healing unusually slowly
- Experiencing more infections than usual

In addition to the symptoms listed above, people with type 1 diabetes may experience nausea, vomiting, or stomach pains. Type 1 diabetes symptoms can develop in just a few weeks or months and the symptoms can be severe.
While the symptoms for type 2 diabetes symptoms are typically those listed above, it is important to note that symptoms often take several years to develop. Some people do not notice any symptoms at all. Because symptoms are hard to spot, it’s important to know the risk factors and to talk with your healthcare providers if you have any of them.
Gestational diabetes (diabetes during pregnancy) also does not typically have any symptoms. If you are pregnant, your provider should be testing you for gestational diabetes between 24 and 28 weeks of pregnancy.
What are the health complications of diabetes?
The long-term health complications of diabetes (also known as diabetes mellitus) develop gradually. The longer you have diabetes, and the less controlled your blood sugar, the higher your risk of complications. Over time, diabetes complications may be disabling or life-threatening.
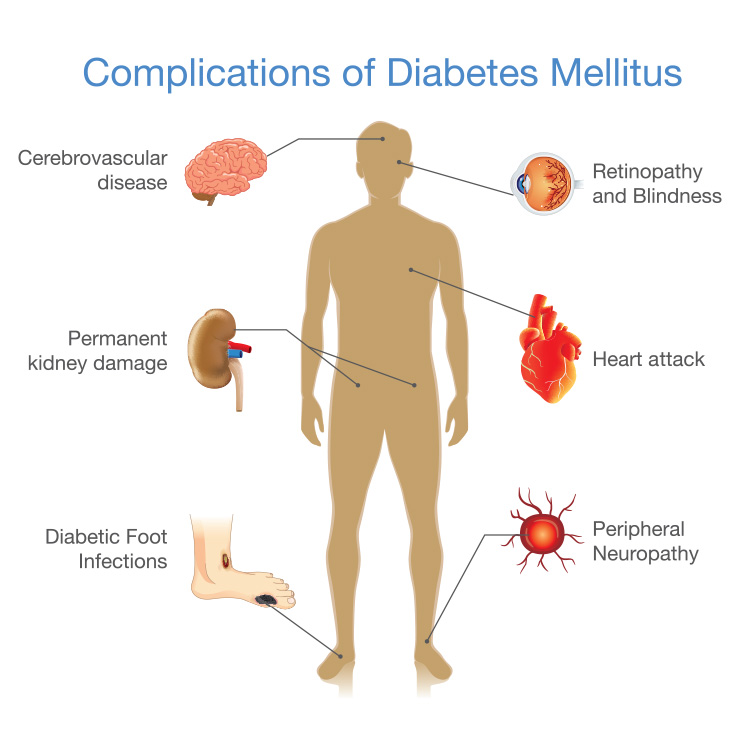
Complications include:
- Cardiovascular disease. Diabetes significantly increases the risk of various cardiovascular complications, including heart attack, stroke, coronary artery disease with chest pain (angina), and narrowing of arteries (atherosclerosis).
- Nerve damage (neuropathy). Excess sugar in your bloodstream can damage the walls of the tiny blood vessels (capillaries) that nourish your nerves, particularly in your legs. This damage can cause tingling, numbness, burning, or pain. The pain usually begins at the tips of toes or fingers and gradually spreads upward. If left untreated, you can lose all sense of feeling in the affected limbs. Damage to the nerves in your intestinal tract can cause problems with nausea, vomiting, diarrhea or constipation. For men, nerve damage can lead to erectile dysfunction.
- Kidney damage (nephropathy). The kidneys contain millions of tiny blood vessel clusters (glomeruli). Glomeruli filter waste from your blood. Diabetes can damage this delicate filtering system. Severe damage can lead to kidney failure or end-stage kidney disease which may require dialysis or a kidney transplant.
- Eye damage (retinopathy). Diabetes can damage the blood vessels of the retina (diabetic retinopathy). This can potentially lead to blindness. Diabetes also increases the risk of other vision conditions, such as cataracts and glaucoma.
- Foot damage. Nerve damage in your feet or poor blood flow to your feet increases the risk of various foot complications. If left untreated, cuts and blisters can develop serious infections, which often heal poorly. These infections may ultimately require toe, foot, or leg amputation.
- Hearing problems. Hearing problems are more common in people with diabetes.
- Skin conditions. Diabetes can leave you more susceptible to skin problems, including bacterial and fungal infections.
- Depression. Depression symptoms are common in people with type 1 and type 2 diabetes and can affect diabetes management. Attention to depression is very important.
Complications Particular to Gestational Diabetes:
Most pregnant women who have gestational diabetes deliver healthy babies. However, if left untreated or uncontrolled, high blood sugar levels can cause problems for both you and your baby.
Complications for your baby include:
- Excess growth. Extra glucose in your bloodstream can cross the placenta, and trigger your baby’s pancreas to make extra insulin. This can cause your baby to grow too large (macrosomia). Large babies are more likely to require a C-section birth.
- Low blood sugar. Sometimes babies of pregnant women with gestational diabetes develop low blood sugar (hypoglycemia) shortly after birth because their own insulin production was high in the womb. This is often addressed with prompt feedings and sometimes an intravenous glucose solution to return the baby’s blood sugar level to normal.
- Type 2 diabetes later in life. Babies of mothers who had gestational diabetes are at higher risk of developing obesity and type 2 diabetes later in their life.
- Death. Untreated gestational diabetes can result in a baby’s death either before or shortly after birth.
Complications for a pregnant woman with gestational diabetes, include:
- Preeclampsia. Preeclampsia is characterized by high blood pressure, swelling in the legs and feets, and a high level of protein in the urine. Preeclampsia can lead to serious or even life-threatening complications for both mother and baby.
- Subsequent gestational diabetes. If you had gestational diabetes in one pregnancy, you are at higher risk to have it again in your next pregnancy. You are also at higher risk to develop diabetes, usually type 2 diabetes, as you get older.
How common is diabetes?
Diabetes is very common in the United States. Approximately 37.3 million American adults (more than 1 in 3) and 1 in 5 of these individuals do not know they have it. The number of adults diagnosed with diabetes has more than doubled in the past 20 years.
- Diabetes is the 7th leading cause of death in the United States
- Diabetes is the #1 cause of kidney failure, adult blindness, and lower-limb amputations
There is not yet a cure for any of the three types of diabetes. Living as healthy a life as possible, taking prescribed medicine as needed, having a strong and supportive healthcare team of both physical and mental healthcare providers, and keeping health care appointments, can all reduce the impact of diabetes on your life.
What is Pre-diabetes?
With pre-diabetes, blood sugar levels are higher than normal, but not yet high enough to be classified as type 2 diabetes. In the United States, more than 1 in 3 people (approximately 96 million) have prediabetes and more than 8 in 10 of these individuals do not know they have it.
Prediabetes significantly raises your risk for type 2 diabetes, heart disease, and stroke. Without proper attention and personal commitment, the likelihood of prediabetes developing into type 2 diabetes is high. The good news about prediabetes, however, is that it can be reversed with the right lifestyle and diet changes.
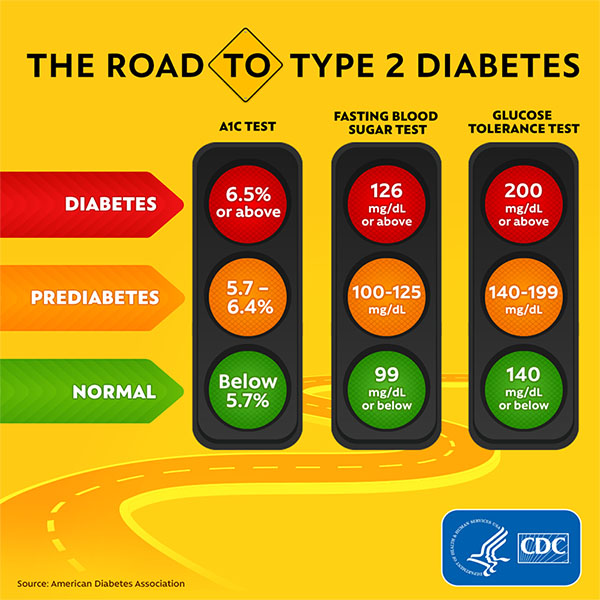
Knowing your A1c levels is the first step to understanding if you are at risk for, or have, diabetes.
The A1c test (also known as the glycated hemoglobin, glycosylated hemoglobin A1C or HbA1c test) is a blood test that measures how much sugar is attached to your blood’s hemoglobin protein. The test gives a measurement of how well your body has controlled the amount of sugar in your bloodstream over the past 2-3 months.
If you already have diabetes, you will do an A1c test every few months to inform you and your healthcare team how well your diabetes management is going and if you need to make any changes in order to improve your management.
Diabetes is a complex and challenging medical condition that requires a team approach. LifeStyle Medical Center is here to partner with you every step of the way.
LifeStyle Medical Centers offers counseling to help prevent diabetes or manage it. Learning how to manage diabetes is a crucial component in living a high quality of life while living with the disease.
Our diabetes treatment services support those with pre-diabetes, type 1 diabetes, type 2 diabetes or gestational diabetes. All types are characterized by high blood glucose (sugar) levels in the blood that result from the body’s inability or ineffectiveness in producing and using insulin, the hormone that helps to control blood glucose levels.
If you think you may have pre-diabetes, type 1 diabetes, type 2 diabetes, or gestational diabetes, consider if you’ve experienced these symptoms:
- Always tired
- Always thirsty
- Always hungry
- Frequent urination
If so, we’re committed to helping you improve your symptoms, reduce your risk of long-term complications and manage your disease. Our team of doctors, nurse practitioners, dietitians and certified diabetes educators are ready to assist you in improving your quality of life by starting our diabetes treatment today.
Call us at (919) 354-7077 or fill out this form to discuss your diabetes prevention or management options.
Sources:
- Centers for Disease Control and Prevention, https://www.cdc.gov/.
- Mayo Clinic, https://www.mayoclinic.org/.
- Johns Hopkins Medicine, https://www.hopkinsmedicine.org/health.
- Cleveland Clinic, https://my.clevelandclinic.org/health/diseases.
